Working Through It: a Leader’s Guide to Building Mentally Healthy Workplaces
Working Through It: a Leader’s Guide to Building Mentally Healthy Workplaces
Before COVID-19, 1 in 5 Canadians experienced a mental health problem or mental illness each year. As the pandemic stretches into 2021, the mental health crisis is following suit.
As a leader, it is important that you recognize where your responsibility to support an employee with a mental health issue begins and ends. You have a responsibility to check-in on your employees, support a psychologically safe culture, and invest in the tools and resources they need to take care of themselves during these uncertain times. You do not have the responsibility to provide the services/support of a medical professional or a trained psychologist, psychiatrist, counsellor, therapist or even friend. Instead, you should be capable of, and willing to, have an honest conversation and refer the employee to appropriate resources.
In support of your role and responsibilities, we’ve put together seven tips for building a mentally healthy workplace, some guidelines for recognizing when your employee requires more help than you/the organization can provide, and some scripts for having that conversation.
As a leader, here’s what you can and should do:
1. Break Down Stigma
Employees often keep silent about mental health struggles, fearing they’ll be viewed differently in the workplace, or worse, face discrimination.
To reduce stigma:
Speak openly about mental illness. Host a company-wide meeting to address pressing challenges, like the pandemic, and the possible impacts on mental health.
Increase your own comfort level and make a habit of talking about stress, depression, anxiety, or other mental illness during check-ins, meetings and e-mail communications. Remind employees that everyone struggles sometimes.
Raise awareness, improve accessibility and encourage use of workplace programs and policies that support mental wellness.
Train managers to identify the signs of mental distress, appropriate ways to assist employees, and indications that medical or mental health professional support is needed.
“When employees trust you won’t call them “crazy” for having a panic attack or fire them when they’re struggling with depression, they’ll be more willing to seek treatment,” says Amy Morin, licensed clinical social worker, psychotherapist and internationally recognized expert on mental strength.
2. Increase your understanding of mental health signs and symptoms
Managers should be trained to recognize signs and symptoms of emotional distress and mental health issues among peers and direct reports and to address them in an appropriate manner. Additionally, “Managers should also listen for frequent and consistent complaints of employee stress. While consistent work stressors may be partly to blame, constant stress is often the ‘face’ of more serious anxiety problems. Verbal admissions of stress are more acceptable for the workplace.
Common Signs of Employee Depression (Shepellfgi.com)
Sad expression
Avoids eye contact
Change in appearance (e.g., weight gain/loss, hygiene, clothes)
Looks tired and fatigued
Depressed speech (i.e., slow, flat, low volume)
Physically agitated (e.g., fidgeting, pacing)
Health complaints (e.g., headache, abdominal and joint pain)
Loses concentration easily
Low interest and morale
Irritable or angry (e.g., outbursts, blaming others)
Frustration over little things
Admissions of guilt and self-blame
Doesn’t contribute or cooperate with others
Isolates self from others
Accidents and mistakes
Absenteeism
Tardiness
Tasks take longer to perform
Lower performance
Alcohol and drug abuse
Of course, in order for managers to detect emotional problems in their employees, they must know what is ‘typical’ behaviour for them. This is why it is crucial for managers to get to know their direct reports as people with characteristic traits, skills, needs and values.”
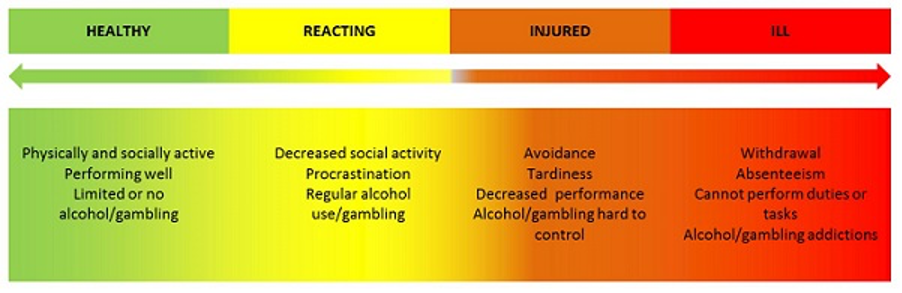
3. Acknowledge That Mental Health is a Spectrum
The Mental Health Continuum Model from the Mental Health Commission of Canada takes away labels and categorizes symptoms of good to poor mental health under a four colour continuum: green (healthy), yellow (reacting), orange (injured), and red (ill).
The colours work well as a stigma reduction tool, allowing employees to talk about mental health neutrally, without labels or diagnoses.
4. Consider Workplace Flexibility and Job Design
Employees need to know that they won’t be penalized for taking care of their mental health. Fortunately, there’s never been a better time to consider flexible work arrangements. Offering mental health days or flexible job design to accommodate therapy appointments or treatment can significantly impact and improve employee mental health, not to mention job satisfaction and productivity.
5. Offer Free Screening Tools
Mental illness often goes untreated because employees don’t recognize the signs and symptoms.
The Canadian Mental Health Association offers a free screening tool that can help employees determine their level of mental fitness. To access the Mental Health Meter, visit https://cmha.ca/mental-health-meter.
6. Develop Mental Health Resources
If you don’t already have a toolbox of resources where employees can find the mental health support they need, consider building one. It doesn’t have to be fancy. Create an intranet page or Google doc of your own resources, use an Employee Assistance Program (EAP), or some combination of the two. And remember, resources only help if employees know about them. Remind your team regularly about the supports available and where to find them.
7. Have a Zero-Tolerance Policy for Harassment and Discrimination
Take a stand against harassment and discrimination. Having the appropriate policies in place makes it clear that these behaviours have no place in your workplace. Ensure that all employees are clear about codes of conduct and the consequences.
More on this topic here:
As a Leader, there is a limit to your responsibility that is met when the issue exceeds your training and your area of expertise. While your own experience and willingness to be an advocate is helpful, you are not expected to, nor should you attempt to do the work of a mental health professional who has undertaken years of education, specialized training and experience to provide appropriate expertise and support.
When the limit of your ability and responsibility has been reached, here are some ideas for addressing mental health with your employees.[i]
An employee indicates concern for their mental health, indicating anxiety, depression, or other issues.
If available, provide them with the contact information for your EAP provider and encourage them to reach out today.
Suggest they connect with their family physician as a starting point. Acknowledge that given current pandemic circumstances, this can take longer than usual!
Provide the distress centre number and encourage them to call to explore alternatives
Encourage them to reach out to a family member or friend and to share their concerns today.
Provide them with the list of resources included at the end of this blog.
What do you say?
“I can see that you’re having a hard time.”
“You don’t seem like yourself – do you want to talk about it?”
“Are you doing ok?”
“Do you have a friend, family member, or therapist that you could call for some support with this?”
“Have you tried connecting with our EAP provider? They have some great resources; I’ll send along their contact information.”
You believe an employee is in crisis, significant distress, or in danger of causing harm to self or others. In no particular order (assess based on situation):
Call the emergency contact listed in their employee file
Refer to an urgent care centre where the can receive an appropriate assessment
Call the police non-emergency line for assistance
Call 911
What do you say?
“We’re going to find someone who can help you”
“I’m going to stay with you (online, on the phone or in person) until we find someone who can help”
Confirm address of current location
Confirm phone number where they can be reached
Confirm the name and contact info for an emergency contact person
Trust your gut. Do not be afraid to overreact. An appropriate exception to confidentiality is a situation where a person is at risk of harm to self or others.
Calgary Community and Urgent Services
Emergency 911
Community Services Line 211
Health Link 811
Distress Centre 403-266-4357. Speak to a highly trained volunteer, who will actively listen and provide additional resources if needed.
24 Hour Crisis line (403) 266-HELP (4357)
24 Hour Teen crisis line (403) 264-8336
E-mail: help@distresscentre.com (not monitored 24 hours a day)
Offered in over 200 languages
Online support via Online crisis chat
Teen specific: CalgaryConnecTeen.com
Text messaging 587-333-2724
Mobile Response Team- access by calling the Distress Centre – 403-266-4357 As an Employer, you can call and receive specific advice when assisting an employee in crisis.
Walk in Counselling:
Urgent Mental Health Services (South Calgary Health Centre (SCHC)/ Sheldon Chumir) or any Hospital Emergency Room
Walk in Counselling at SCHC (evenings 4-7 pm) no appointment needed 403-943-9374
Eastside Family Centre –no appointment needed- (11 am- 7pm) 403-299-9696
Access Mental Health (Alberta Health Services) Information 403-943-1500
Alberta Health Services Mental Health Help Line. Call 1-877-303-2642.
Canadian Mental Health and Suicide Services 403-297-1708
Addictions (Alberta Health Services) 403-367-5000
Addiction Services Helpline – 1-866-332-2322 – 24 Hours
Bullying Helpline – bullyfreealberta.ca 1-888-456-2323 – 24 Hours
Child Abuse Hotline – 1-800-387-5437 – 24 Hours
Family Violence Info Line – 310-1818 – 24 Hours
Income Support Contact Centre – Financial help for Albertans who don’t have resources to meet their basic needs (e.g., food, clothing, shelter) 1-866-644-5135 – 24 Hours
Kids Help Phone – kidshelpphone.ca – 1-800-668-6868 – 24 Hours
Medication & Herbal Advice Line – 1-800-332-1414 – 24 Hours
Mental Health Helpline – 1-877-303-2642 – 24 Hours
Poison & Drug Information service – 1-800-332-1414 – 24 Hours
CIWA (Calgary Immigrant Women’s Assoc.) https://www.ciwa-online.com/ 403-263-4414
Domestic Violence
Calgary Women’s Emergency (family violence hotline) 403-234-7233
Sheriff King 403-237-5888 -YWCA of Calgary- 403-266-4111 or 403-266-0707
Calgary Communities Against Sexual Abuse (CCASA) 403-237-5888
Hospice Calgary- Children’s Grief Centre 403-263-4525
AHS Grief Support Program 403-955-8011
Woods Homes Youth Community Response Team 403-299-9699 or 1-800-563-6106. Text 587-315-5000 between 9 a.m. and 10 p.m. Find information on no-cost walk-in counselling services.
Kerby Center (ages 65+) 403-265-0661
Calgary Counselling Centre 833-827-4229
Calgary Family Therapy Program 403-802-1680
CARYA -Individual and family 403-269-9888 – Family Support and Services
Catholic Family Services 403-233-2360
YWCA Counselling 403-536-2844
Wellness Together Canada – helps connect you to mental health and substance use support, resources, and counselling with a mental health professional. (https://ca.portal.gs/)
Metis Nation of Alberta (http://albertametis.com/covid-19-information/mental-health/)
Social-Emotional Learning Government Resource (https://www.alberta.ca/social-emotional-learning.aspx)
Trauma-informed practice Government Resource (https://www.alberta.ca/trauma-informed-practice.aspx)
Working Together to Support Mental Health in Alberta Schools (https://education.alberta.ca/media/3576206/working_together_to_support_mental_health.pdf)
Alberta Community of Social Service – Children’s Mental Health Government Resource (https://www.alberta.ca/childrens-mental-health.aspx)
Community Connect YYC – Book affordable barrier-free phone or video counselling sessions. https://www.communityconnectyyc.ca/
Togetherall – Join and connect to a clinically moderated online peer-to-peer mental health community. – Free to Albertans over the age of 16. https://togetherall.com/en-ca/
Bounceback – A free guided self-help program that helps adults and youth age 15-plus learn how to manage low mood, mild-to-moderate depression, anxiety, stress or worry. https://bouncebackbc.ca/
Wellness Together Canada – Free online resources and supports, including immediate text support, information and videos, self-guided mental wellness programs and counselling. https://ca.portal.gs/
PRIVATE COUNSELLING OPTIONS- FEE for SERVICE- Practitioners can be found on The Psychology Today, ACSW, Alberta Psychologists or Accelerated Resolution Therapy Website.
Creating psychologically safe and healthy workplaces is a subject that we care about a lot at Cenera. Our HR Advisors welcome the opportunity to discuss how we can help you build a safer, healthier workplace now and into the future.
Contact us today to book a consultation!
Let’s Connect
Never miss an update, click here to subscribe to our monthly newsletter.
Plus, follow us on LinkedIn!
Share This Story, and Choose Your Platform!